Patellar Fracture
Updated:
(Also known as Fractured Patella, Fractured Knee Cap)
What is a patellar fracture?
A patellar fracture is a condition characterized by a break in the knee cap bone (patella) (figure 1).
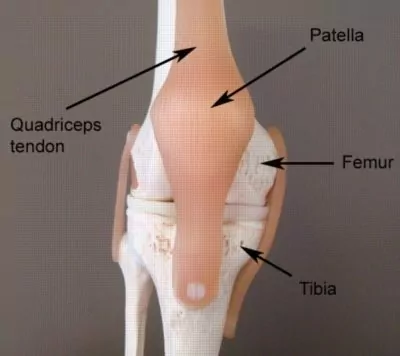
The knee comprises of the union of 3 bones – the long bone of the thigh (femur), the shin bone (tibia) and the knee cap (patella) (figure 1). The patella (knee cap) is situated at the front of the knee and lies within the tendon of the quadriceps muscle (the muscle at the front of the thigh). The quadriceps tendon envelops the patella and attaches to the top end of the tibia (figure 1). Due to this relationship, the knee cap sits in front of the femur forming a joint in which the bones are almost in contact with each other.
During certain activities, such as a fall onto the knee cap or following a direct blow to the front of the knee, stress is placed on the patella bone. When this stress is traumatic, and beyond what the bone can withstand, a break in the patella may occur. This condition is known as a patellar fracture.
Because of the large forces required to break the patella bone, a patellar fracture often occurs in combination with other injuries such as patellofemoral joint damage or a quadriceps tear.
Patellar fractures can vary in location, severity and type including stress fracture, displaced fracture, un-displaced fracture, compound fracture, greenstick, comminuted etc.
Causes of a patellar fracture
A patellar fracture most commonly occurs due to direct trauma to the knee cap such as a fall onto the knee cap or a direct blow to the patella (e.g. from a hockey stick). Occasionally it may also occur due to a forceful quadriceps contraction such as landing from a height. A stress fracture to the patella, although rare, may occur as a result of overuse, often associated with a recent increase or high volume of jumping. An acute patellar dislocation can also sometimes result in a fracture to the patella.
Signs and symptoms of a patellar fracture
Patients with this condition typically experience a sudden onset of sharp, intense pain at the front of the knee at the time of injury. This often causes the patient to limp so as to protect the patella. In severe cases, particularly involving a displaced fracture of the patella, weight bearing may be impossible. Pain is usually felt on the front or sides of the patella and can occasionally settle quickly with rest leaving patients with an ache at the site of injury that may be particularly prominent at night or first thing in the morning. Occasionally patients may experience symptoms in the back of the knee, the thigh or lower leg regions.
Patients with a patellar fracture may also experience swelling, bruising and pain on firmly touching the affected region of bone. Pain may also increase during certain movements of the knee when standing or walking (particularly up or down hills or on uneven surfaces) or when attempting to stand or walk. Squatting or kneeling is also usually painful with many patients being unable to perform these activities. In severe cases (with bony displacement), an obvious deformity may be noticeable. Occasionally patients may also experience pins and needles or numbness in the knee, lower leg, foot or ankle.
Diagnosis of a patellar fracture
A thorough subjective and objective examination from a physiotherapist is essential to assist with diagnosis of a patellar fracture. X-rays (including a skyline view of the patella) are usually required to confirm diagnosis and assess the severity of the fracture. Further investigations such as an MRI, CT scan or bone scan may be required, in some cases, to assist with diagnosis and assess the severity of the injury.
Treatment for a patellar fracture

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Prognosis of a patellar fracture
Patients with this condition usually make a full recovery with appropriate management (whether surgical or conservative). Return to activity or sport can usually take place in a number of weeks to many months and should be guided by the treating physiotherapist and specialist. In patients with severe injuries such as those that involve damage to other bones, soft tissue, nerves or blood vessels, recovery time may be significantly prolonged and there may be some ongoing disability.
Sometimes a poorly rehabilitated patellar fracture may develop into other conditions such as patellofemoral pain syndrome even though full bony healing may have taken place. In these instances further physiotherapy treatment and rehabilitation may be required before the patient is able to return to full activity, pain free.
Physiotherapy for a patellar fracture
Physiotherapy treatment is vital in all patients with this condition to hasten healing and ensure an optimal outcome. Treatment may comprise:
- soft tissue massage
- joint mobilization
- electrotherapy (e.g. ultrasound)
- dry needling
- patella taping or bracing
- the use of a protective splint
- ice or heat treatment
- the use of crutches
- progressive exercises to improve strength (especially the quadriceps VMO muscle), flexibility, core stability and balance
- hydrotherapy
- education
- activity modification
- a graduated return to activity plan
- biomechanical correction
- footwear advice
Other intervention for a patellar fracture
Despite appropriate physiotherapy management, some patients with this condition do not improve adequately and may require other intervention. The treating physiotherapist or doctor can advise on the best course of management when this is the case. This may include further investigations such as X-rays, CT scan, MRI or bone scan, periods of splinting or plaster cast immobilization or referral to appropriate medical authorities who can advise on any intervention that may be appropriate to improve the fractured patella. Occasionally, patients with fractures that are initially managed without surgical intervention may require surgery to stabilize the fracture and a bone graft to aid fracture healing.
Exercises for a patellar fracture
The following exercises are commonly prescribed to patients with a patellar fracture following confirmation that the fracture has healed or that pain free mobilization can commence as directed by the surgeon. You should discuss the suitability of these exercises with your physiotherapist prior to beginning them. Generally, they should be performed 3 times daily and only provided they do not cause or increase symptoms.
Your physiotherapist can advise when it is appropriate to begin the initial exercises and eventually progress to the intermediate, advanced and other exercises. As a general rule, addition of exercises should take place provided there is no increase in symptoms.
Initial Exercises
Static Quadriceps Contraction
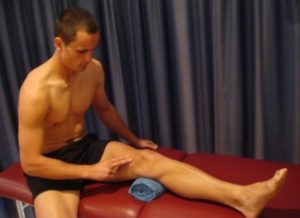
Tighten the muscle at the front of your thigh (quadriceps) by pushing your knee down into a towel (figure 2). Put your fingers on your inner quadriceps to feel the muscle tighten during contraction. Hold for 5 seconds and repeat 10 times as hard as possible without increasing your symptoms.
Knee Bend to Straighten
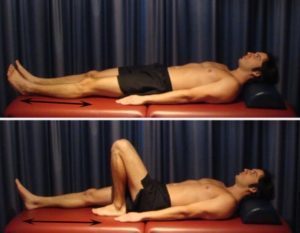
Bend and straighten your knee as far as you can go without pain and provided you feel no more than a mild to moderate stretch (figure 3). Gradually increase movement as tolerated over a number of sessions provided the exercise is pain free. Repeat 10 – 20 times provided there is no increase in symptoms.
Hip Extension in Standing
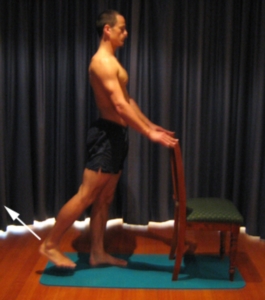
Begin this exercise standing at a table or bench for balance. Keeping your back and knee straight, slowly take your leg backwards, tightening your bottom muscles (gluteals) (figure 4). Hold for 2 seconds then slowly return to the starting position. Repeat 10 times provided the exercise is pain free.
Intermediate Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Advanced Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Other Exercises

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
Rehabilitation protocol for patellar fracture

Members Only ContentBecome a PhysioAdvisor Member to gain full access to this exclusive content. For more details see Become a Member. Already a member? Login Now
 Find a Physio
Find a Physio
Find a Physiotherapist in your local area who can treat this condition.
 More Exercises
More Exercises
- View more Knee Strengthening Exercises.
- View more Knee Flexibility Exercises.
- View more Balance Exercises.
- View more Leg Stretches.
- View more Leg Strengthening Exercises.
 Physiotherapy products for a patellar fracture
Physiotherapy products for a patellar fracture
Some of the most commonly recommended products by physiotherapists to hasten healing and speed recovery in patients with this condition include:
-
 AllCare Ortho Patella Tracker (AOK28)
AllCare Ortho Patella Tracker (AOK28) -
 AllCare Ortho – Tri-Panel Knee Immobiliser (AOK81)
AllCare Ortho – Tri-Panel Knee Immobiliser (AOK81) -
 Forearm Crutches Adjustable – Standard Grip
Forearm Crutches Adjustable – Standard Grip -
 AllCare Band
AllCare Band -
 Premium Strapping Tape 38mm (Victor)
Premium Strapping Tape 38mm (Victor) -
 AllCare Tubing
AllCare Tubing -
 AllCare Spikey Massage Ball
AllCare Spikey Massage Ball -
 Mueller Hinged Knee Brace
Mueller Hinged Knee Brace -
 Fixomull Stretch 5cm x 10m
Fixomull Stretch 5cm x 10m -
 AllCare Instant Cold Pack (15 x 25cm)
AllCare Instant Cold Pack (15 x 25cm) -
 AllCare Foam Roller Round
AllCare Foam Roller Round
To purchase physiotherapy products for a fractured patellar click on one of the above links or visit the PhysioAdvisor Shop.
 More Information
More Information
- View detailed information on initial injury management and the R.I.C.E. Regime.
- View detailed information on How to use Crutches.
- View detailed information on when to use Ice or Heat.
- View detailed information on a Return to Running Program.
- View detailed information on how to safely Return to Sport.
- View detailed information on Patella Taping.
- Unsure of your most likely diagnosis? View our Knee Diagnosis Guide.
Become a PhysioAdvisor Member
-
 Individual Membership (12 Months)$59.95 for 1 year
Individual Membership (12 Months)$59.95 for 1 year -
 Individual Membership (3 Months)$39.95 for 3 months
Individual Membership (3 Months)$39.95 for 3 months -
 Individual Membership (Yearly)$49.95 / year
Individual Membership (Yearly)$49.95 / year -
 Individual Membership (Monthly)$15.95 / month
Individual Membership (Monthly)$15.95 / month

Link to this Page
If you would like to link to this article on your website, simply copy the code below and add it to your page:
<a href="https://physioadvisor.com.au/injuries/knee/patellar-fracture”>Patellar Fracture – PhysioAdvisor.com</a><br/>PhysioAdvisor offers detailed physiotherapy information on a patellar fracture including: diagnosis, treatment, exercises, physiotherapy products and more...
Return to the top of Patellar Fracture.
