Pre-Patellar Bursitis
Updated:
(Also known as Housemaid’s Knee, Patellar Bursitis)
What is pre-patellar bursitis?
Pre-patellar bursitis is a condition characterized by tissue damage and inflammation of the pre-patellar bursa (a small fluid filled sac located between the knee cap and skin) causing pain in the front of the knee.
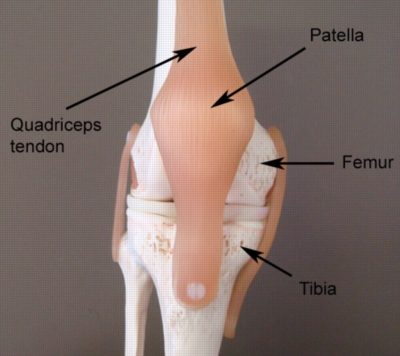
The knee comprises of the union of 3 bones – the long bone of the thigh (femur), the shin bone (tibia) and the knee cap (patella) (figure 1). The patella (knee cap) is situated at the front of the knee. Between the knee cap and the overlying skin lies the pre-patellar bursa (figure 2). A bursa is a small sac filled with lubricating fluid and is designed to reduce friction between adjacent soft tissue or bony layers. The pre-patellar bursa reduces friction between the knee cap and the overlying skin.
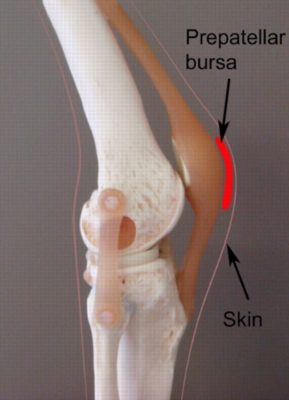
During kneeling, compressive forces are placed through the pre-patellar bursa. Pressure may also be placed on the pre-patellar bursa following a direct impact or fall onto the knee cap. When these forces are excessive due to too much repetition or high force, irritation and inflammation of the bursa may occur. When this occurs, the condition is known as pre-patellar bursitis.
Causes of pre-patellar bursitis
Pre-patellar bursitis most commonly occurs due to repetitive or prolonged activities placing strain on the pre-patellar bursa. This typically occurs due to repetitive or prolonged kneeling especially on hard surfaces. Occasionally, the condition may occur suddenly due a direct blow to the front of the knee or due to a fall onto the knee cap. In rare cases, pre-patellar bursitis may be caused by an infection associated with a cut in the front of the knee or recent knee surgery.
Signs and symptoms of pre-patellar bursitis
Patients with pre-patellar bursitis typically experience pain and swelling that develops gradually at the front of the knee directly in front of the knee cap. Swelling is usually obvious as the bursa lies directly beneath the skin. In less severe cases, patients may only experience an ache or stiffness in the knee that increases with rest following activities placing strain on the pre-patellar bursa (such as kneeling). The pain associated with this condition may also warm up (or feel better) with activity in the initial stages of the condition. As the condition progresses, patients may experience symptoms that increase during activity affecting performance. Other symptoms may include reduced knee range of movement, pain on firmly touching the pre-patellar bursa (figure 2) and, in some cases, pain or a limp may be present when walking (particularly up hills or on uneven surfaces).
Diagnosis of pre-patellar bursitis
A thorough subjective and objective examination from a physiotherapist is usually sufficient to diagnose pre-patellar bursitis. Occasionally, further investigations such as an Ultrasound, X-ray, MRI, CT scan or blood test may be required to rule out other conditions, assist with diagnosis and assess the severity of the condition.
Treatment for pre-patellar bursitis
Most cases of pre-patellar bursitis settle with appropriate physiotherapy. The success rate of treatment is largely dictated by patient compliance. One of the key components of treatment is that the patient rests sufficiently from any activity that increases their pain until they are symptom free. Activities which place large amounts of stress on the pre-patellar bursa should also be minimized particularly kneeling or direct impact to the front of the knee. Rest from aggravating activities allows the body to begin the healing process in the absence of further tissue damage. Once the patient can perform these activities pain free, a gradual return to these activities is indicated provided there is no increase in symptoms. Ignoring symptoms or adopting a ‘no pain, no gain’ attitude is likely to lead to the condition becoming chronic. Immediate, appropriate treatment in all patients with pre-patellar bursitis is essential to ensure a speedy recovery. Once the condition is chronic, healing slows significantly resulting in markedly increased recovery times and an increased likelihood of future recurrence.
Patients with pre-patellar bursitis should follow the R.I.C.E. Regime in the initial phase of injury. The R.I.C.E regime is beneficial in the first 72 hours following injury or when inflammatory signs are present (i.e. morning pain, night pain or pain with rest). The R.I.C.E. regime involves resting from aggravating activities, regular icing, the use of a compression bandage and keeping the affected leg elevated above the level of your heart. Anti-inflammatory medication may also hasten the healing process by reducing the pain and swelling associated with inflammation.
Manual “hands-on” treatment from a physiotherapist, such as massage, trigger point release techniques, dry needling, joint mobilisation, stretches and electrotherapy, can assist with improving range of movement, pain and function, and assist with hastening return to activity.
In severe cases of pre-patellar bursitis or those that are unresponsive to physiotherapy, aspiration (drainage) and infiltration of the bursa with a corticosteroid and anesthetic may be required. This is usually followed by the use of a firm compression bandage and a period of rest (usually 48 hours). Patients with this condition should perform pain free flexibility and strengthening exercises as part of their rehabilitation to ensure an optimal outcome. The treating physiotherapist can advise which exercises are most appropriate for the patient and when they should be commenced. In the final stages of rehabilitation, a graduated return to running or activity program is required to recondition the bursa to running or activity in a safe and effective manner. This should include the implementation of progressive acceleration and deceleration running drills before returning to sport and should be guided by the treating physiotherapist.
Prognosis of pre-patellar bursitis
With appropriate management and physiotherapy treatment, most minor cases of pre-patellar bursitis usually recover and return to normal function in a number of weeks. In more severe and / or chronic cases, rehabilitation may be significantly longer and other intervention such as a corticosteroid injection may be required to ensure an optimal outcome. Early physiotherapy intervention is vital to hasten recovery in all patients with this condition.
Physiotherapy for pre-patellar bursitis
Physiotherapy treatment for pre-patellar bursitis is vital to hasten the healing process, ensure an optimal outcome and reduce the likelihood of injury recurrence. Treatment may comprise:
- soft tissue massage
- electrotherapy (e.g. ultrasound)
- joint mobilization
- ice treatment
- exercises to improve knee strength and flexibility
- the use of crutches
- the use of knee pads for kneeling
- education
- anti-inflammatory advice
- activity modification advice
- a graduated return to activity program
Other intervention for pre-patellar bursitis
Despite appropriate physiotherapy management, some patients with pre-patellar bursitis do not improve adequately. When this occurs the treating physiotherapist or doctor will advise on the best course of management. This may include further investigations such as X-rays, ultrasound, MRI or CT scan, blood tests, pharmaceutical intervention, bursa aspiration, corticosteroid and anesthetic injection, or referral to appropriate medical authorities who can advise on any interventions that may be appropriate to improve the condition. In rare cases that are unresponsive to conservative measures surgical intervention may be required to remove the pre-patellar bursa.
Exercises for pre-patellar bursitis
The following exercises are commonly prescribed to patients with this pre-patellar bursitis. You should discuss the suitability of these exercises with your physiotherapist prior to beginning them. Generally, they should be performed 1 – 3 times daily and only provided they do not cause or increase symptoms.
Static Inner Quadriceps Contraction
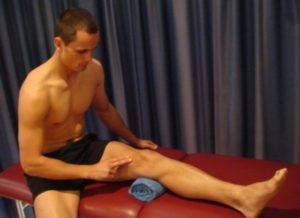
Tighten the muscle at the front of your thigh (quadriceps) by pushing your knee down into a small towel (figure 3). Put your fingers on your inner quadriceps (vastus medialis) to feel the muscle tighten during contraction. Hold for 5 seconds and repeat 10 times as hard as possible provided the exercise is pain free.
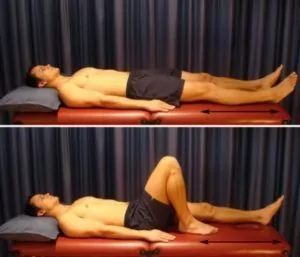
Knee Bend to Straighten
Bend and straighten your knee as far as possible without increasing your pain (figure 4). Repeat 10 – 20 times provided there is no increase in symptoms.
Physiotherapy products for pre-patellar bursitis
Some of the most commonly recommended products by physiotherapists to hasten healing and speed recovery in patients with pre-patellar bursitis include:
To purchase physiotherapy products for pre-patellar bursitis click on one of the above links or visit the PhysioAdvisor Shop.
Find a Physio for pre-patellar bursitis
Find a physiotherapist in your local area who can treat pre-patellar bursitis.
Other Exercises
- View Knee Stretches
- View more Knee Strengthening Exercises

Link to this Page
If you would like to link to this article on your website, simply copy the code below and add it to your page:
<a href="https://physioadvisor.com.au/injuries/knee/prepatellar-bursitis”>Pre-Patellar Bursitis – PhysioAdvisor.com</a><br/>PhysioAdvisor offers detailed physiotherapy information on Pre-Patellar Bursitis (Housemaid's Knee) including signs and symptoms, diagnosis, treatment, exercises and more...
Return to the top of Pre-Patellar Bursitis.