Compartment Syndrome (Deep Posterior)
Updated:
(Also known as Deep Posterior Compartment Syndrome)
What is compartment syndrome?
Compartment syndrome is a condition characterized by a variety of symptoms (such as pain and muscle tightness) which occur in the lower leg as a result of exercise-induced muscle swelling and a subsequent increase in local tissue pressure.
There are several muscles which lie at the back of the lower leg and are collectively known as the calf muscles (figure 1). Several of these muscles lie deep within the calf (flexor hallicus longus, flexor digitorum longus and tibialis posterior) and are enveloped in a layer of connective tissue (fascia) which encloses them, therefore forming a compartment. This compartment is known as the deep posterior compartment.
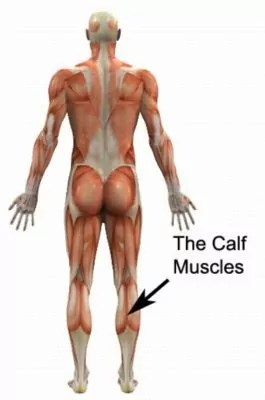
Occasionally, the compartments’ enveloping layer of connective tissue becomes tight and inflexible resulting in an increase in pressure within the compartment. This may be due to an inflammatory process whereby the connective tissue loses its elasticity. In addition, activity requiring repeated use of muscles within the deep posterior compartment (such as running) results in a local increase in blood flow, causing the muscles to swell. Subsequently, the pressure within the compartment may increase excessively during activity resulting in a variety of lower leg symptoms such as tightness, pain, weakness, pins and needles or numbness. When this occurs, the condition is known as deep posterior compartment syndrome.
Occasionally, compartment syndrome may occur in combination with other conditions that cause shin pain such as shin splints and stress fractures.
Causes of compartment syndrome
Compartment syndrome is usually associated with overuse (such as a sudden increase in training or running) and is often seen in runners and footballers. It frequently occurs in association with calf muscle tightness, an increase in calf muscle size or biomechanical abnormalities, such as excessive pronation (flat feet – figure 2) or, less commonly, supination (high arch). Patients often develop this condition early in the season following a period of reduced activity (deconditioning) and when training surfaces are generally harder.
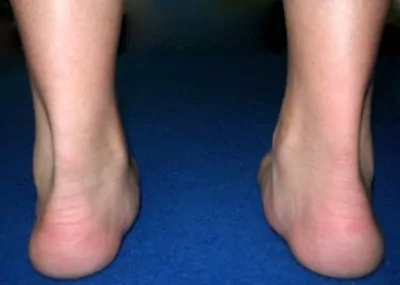
Signs and symptoms of compartment syndrome
Patients with deep posterior compartment syndrome typically experience pain and tightness along the inner aspect of the shin and / or back of the lower leg. Symptoms generally increase with exercise and decrease with rest and can occur in one or both legs.
Patients with this condition may experience an ache, tightness or bursting sensation that can progress to chronic calf pain with excessive activity. In severe cases, patients may experience weakness, pins and needles in the foot, numbness or a ‘dead’ feeling in the leg that develops with ongoing activity. Usually symptoms will disappear relatively quickly upon resting.
Patients usually do not experience pain on firmly touching the affected area, however, if other conditions are present, such as shin splints, there may be tenderness along the inner border of the shin bone. Areas of muscle tightness, thickening or lumps may also be detected in the area of pain.
Diagnosis of compartment syndrome
A thorough subjective and objective examination from a physiotherapist is usually sufficient to diagnose compartment syndrome. Compartment pressure testing can be used to confirm the diagnosis and identify the exact muscle compartment involved. Investigations such as an X-ray, bone scan, CT scan or MRI may sometimes also be used to assist with diagnosis and exclude the presence of other pathologies.
Treatment for compartment syndrome
Most cases of compartment syndrome settle well with appropriate physiotherapy. This requires careful assessment by the physiotherapist to determine which factors have contributed to the development of the condition, with subsequent correction of these factors. Soft tissue massage and stretches to address muscle tightness play a large role in treatment, along with biomechanical assessment and correction to address any foot posture issues.
The success rate of treatment for patients with this condition is largely dictated by patient compliance. One of the key components of treatment is that the patient rests sufficiently from ANY activity that increases their pain until they are symptom free. Once pain free, a gradual return to activity is indicated provided there is no increase in symptoms.
Ignoring symptoms or adopting a ‘no pain, no gain’ attitude is likely to lead to the problem becoming chronic. Immediate, appropriate treatment in patients with compartment syndrome is essential to ensure a speedy recovery. Once the condition is chronic, healing slows significantly resulting in markedly increased recovery times.
Activities placing minimal stress on the lower leg may be performed to maintain fitness. These include hydrotherapy exercises or swimming in a pool, upper body weights in sitting or lying or sometimes cycling.
Deep tissue massage to the calf muscles can be a very effective way of treating compartment syndrome and should form part of the rehabilitation program. Patients should also perform pain-free flexibility and strengthening exercises as part of their rehabilitation to ensure an optimal outcome.
In the final stages of treatment, once pain has been controlled and contributing factors have been addressed, a graduated return to activity or sport can occur as guided by a physiotherapist.
If conservative treatment fails, surgery may be indicated to reduce the pressure within the muscle compartment. This procedure involves removal of the connective tissue surrounding the muscles to allow greater room for the muscles to swell during activity without causing symptoms.
Prognosis of compartment syndrome
Most patients with compartment syndrome can recover with appropriate treatment. Recovery time may range from a few weeks to many months depending on the severity of injury, quality of treatment and length of time the injury has been present for. Patients with compartment syndrome that have been present for months may require a considerable period of treatment associated with reduced activity before full recovery can occur.
Contributing factors to the development of compartment syndrome
There are several factors which can predispose patients to developing compartment syndrome. These need to be assessed and corrected with direction from a physiotherapist. Some of these factors include:
- excessive training or activity
- poor foot posture (especially flat feet)
- inappropriate footwear
- training on hard surfaces
- muscle weakness (especially the calf muscles)
- tightness in specific joints (such as the ankle)
- tightness in specific muscles (especially the deep calf muscles)
- muscle strength imbalances
- an increase in calf muscle size
- poor lower limb biomechanics
- poor training technique or methods
- leg length differences
- being overweight
- deconditioning
- fatigue
- past injury or scarring to the fascia
Physiotherapy for compartment syndrome
Physiotherapy treatment for compartment syndrome is vital to ensure an optimal outcome. Treatment may comprise:
- soft tissue massage (particularly to the deep calf muscles)
- mobilization (of the ankle joint)
- dry needling
- electrotherapy
- PNF stretches
- arch support taping
- the use of orthotics
- biomechanical correction
- progressive exercises to improve flexibility (especially of the deep calf muscles), balance and strength
- activity modification advice
- footwear advice
- weight loss advice where appropriate
- a gradual return to activity program
Other intervention for compartment syndrome
Despite appropriate physiotherapy management, some patients with compartment syndrome do not improve. When this occurs the treating physiotherapist or doctor can advise on the best course of management. This may include further investigations such as X-rays, bone scan, CT scan, MRI, or compartment pressure testing, or a referral to an orthopaedic specialist. In the event that conservative treatment has failed, and, compartment pressure testing is positive, surgery may be indicated to reduce the pressure within the compartment. A review with a podiatrist may also be indicated for the prescription of orthotics to correct any foot posture abnormalities.
Exercises for compartment syndrome
The following exercises are commonly prescribed to patients with this condition. You should discuss the suitability of these exercises with your physiotherapist prior to beginning them. Generally, they should be performed 3 times daily and only provided they do not cause or increase symptoms.
Lunge Stretch
With your hands against the wall, place your leg to be stretched in front of you as demonstrated (figure 3). Keep your heel down. Gently move your knee forward over your toes until you feel a stretch in the back of your calf or Achilles tendon. Hold for 15 seconds and repeat 4 times at a mild to moderate stretch pain-free.

Calf Stretch
With your hands against the wall, place your leg to be stretched behind you as demonstrated (figure 4). Keep your heel down, knee straight and feet pointing forwards. Gently lunge forwards until you feel a stretch in your calf / knee of your back leg. Hold for 15 seconds and repeat 4 times at a mild to moderate stretch pain-free.

Physiotherapy products for compartment syndrome
Some of the most commonly recommended products by physiotherapists to hasten healing and speed recovery in patients with this condition include:
- Massage Balls & Foam Rollers (for self massage)
- Ice Packs or Heat Packs
To purchase physiotherapy products for compartment syndrome click on one of the above links or visit the PhysioAdvisor Shop.
Find a Physio for compartment syndrome
Find a physiotherapist in your local area who can treat this condition.
Other Exercises
- View more Calf Flexibility Exercises.
- View Calf Strengthening Exercises.
- View Balance Exercises.
Further Information
- Learn more about Correct Footwear for Running.
- Read about Shin Splints.

Link to this Page
If you would like to link to this article on your website, simply copy the code below and add it to your page:
<a href="https://physioadvisor.com.au/injuries/lower-leg/compartment-syndrome-deep-posterior”>Compartment Syndrome (Deep Posterior) – PhysioAdvisor.com</a><br/>PhysioAdvisor offers detailed physiotherapy information on compartment syndrome including: signs and symptoms, causes, diagnosis, treatment, exercises, physiotherapy products and more...
Return to the top of Compartment Syndrome (Deep Posterior).
